Keratoconus is a degenerative disorder of the eye in which structural changes occur within the cornea cause it to thin and change to a more conical shape. It is a progressive condition that often develops in a person’s teenage years and advances in their early adulthood, gradually worsening overtime.
Keratoconus is not associated with physical symptoms such as inflammation and redness; therefore, this condition may go undetected for a long period of time. Although it commonly affects both eyes, individuals with keratoconus typically notice their vision deteriorating in one eye and gradually to the next eye.
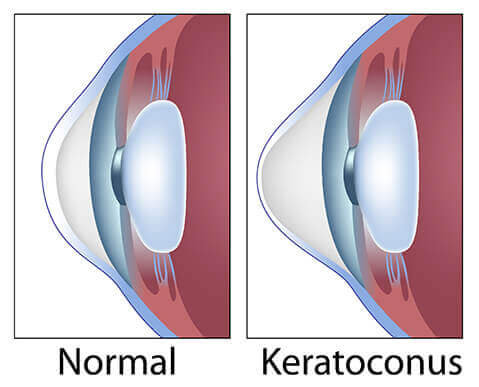
Environmental and genetic factors are considered possible causes, but the exact cause is uncertain. The cornea of the eye is composed of tiny fibers of proteins called collagen. In a patient with keratoconus those fibers become weak, and they are no longer able to hold the normal cornea curvature. As keratoconus progresses the cornea becomes increasingly irregular in shape.
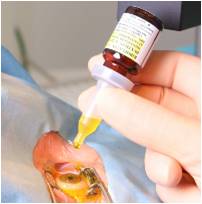
The aim of this treatment is to arrest progression of keratoconus, and thereby prevent further deterioration in vision and the possible need for corneal transplantation. During the corneal collagen cross-linking treatment, custom-made riboflavin drops saturate the cornea, which is then activated by ultraviolet light. This process has been shown in laboratory and clinical studies to increase the amount of collagen cross-linking in the cornea and strengthen the cornea.


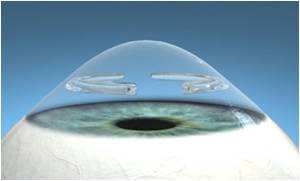
Intacs serve as a possible treatment option for patients with keratoconus that are experiencing intolerance to their contact lenses. The Intacs (corneal implants) have been proven to stabilize the cornea, improve vision, provide the possibility for a more successful contact lens fitting, and potentially defer the need for a corneal transplant. The intracorneal segments effectively cause redistribution of corneal curvature that reduces astigmatism and improves visual acuity.
The need for glasses or contact lenses will still be needed following the cross-linking treatment and/or implantation of intracorneal ring segments.


Rigid gas permeable lenses are designed to comfortably sit on top of the cone shaped cornea. The lens creates a new refractive surface while providing substantial lubrication at the space in between the front of the eye and the lens. Specialty design keratoconic lenses are available and may be a more comfortable option depending on the severity of the condition.
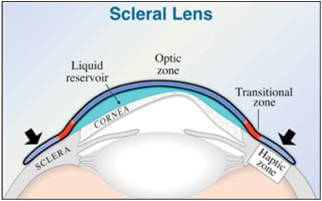
Evolutionary lens designs and materials in scleral contact lenses have made it possible to improve visual acuity for patients that struggled to achieve adequate vision in previous contact lens options. A scleral lens is a large diameter lens that rest on the white part of the eye, called the sclera, and the lens vaults completely over the cornea. Because of their size, the sclera lenses do not fall out and dust or dirt particles cannot get under them during wear. They are surprisingly comfortable to wear because the edges of the lens rests above and below the eye lid margins so there is no lens awareness.
If you are experiencing keratoconus, our Houston keratoconus eye doctors at Mann Eye Institute and Laser Centers will guide you in the best direction for your treatment options! Call Mann Eye Institute to schedule a consultation today and to learn more about our surgical and specialty lens options for keratoconus!
AvaGen™ is the genetic eye test that provides answers on your risk for keratoconus and other corneal diseases—helping you and your doctor make confident eye care decisions now. The unique AvaGen™ test is:

Keratoconus and corneal dystrophies progressively worsen over time if left untreated. In the past, these conditions often went undiagnosed until they permanently affected vision. Now, AvaGen™ can help your doctor take immediate actions to help protect and preserve your vision or to evaluate treatment decisions, including whether or not you can undergo vision-correcting procedures such as LASIK.
With AvaGen™, you will have the peace of mind of knowing you’re doing the utmost to protect your vision.
After a simple, in-office cheek swab to gather a DNA sample, the test is sent to a special lab for analysis. Your doctor will inform you of the results, answer questions, and discuss potential next steps. A genetic counselor can further explain what the results mean for your vision, and what to expect next.
Schedule a consultation today to learn more about genetic testing for keratoconus at Mann Eye Institute.
The Mann Eye Institute is a leading eye care facility with sixteen locations in Humble, West Humble, Houston, Central Austin, North Austin, Sugar Land, Katy, Spring, The Woodlands, Livingston, Bay City, Pearland, Baytown, Tomball, Sun City, and Cleveland, Texas. With various locations in the Houston and Austin areas we can provide the full continuum of care, including; designer eyewear and eye care needs, LASIK eye surgery, cataract surgery, premium lens implants and dry eye treatment options. If you are seeking expert eye doctors in Texas contact us today!
The Woodlands Office
Medical Arts Center III
17450 St. Luke’s Way, Suite 100
The Woodlands, TX 77384
(281) 367-2010
Pearland Office
10223 Broadway St., Ste. J
Pearland, TX 77584
(281) 971-9332
Spring Office
2616 FM 2920 Ste. I
Spring, TX 77388
(281) 353-8300
Tomball Office
14079 FM 2920
Tomball, TX 77377
(346) 701-4029
Katy Office
750 Westgreen Blvd.
Katy, TX 77450
(281) 392-3937
Humble - Deerbrook Office
9802 FM 1960 W, Ste. 110
Humble, Texas 77338
(281) 446-9333
Sugar Land Office
6424 E. Riverpark Dr.
Sugar Land, TX 77479
(713) 580-2525
Humble - S. Memorial Office
18850 S. Memorial Blvd.
Humble, TX 77338
(281) 446-7900
Livingston Office
1601 US-59 Loop North, Ste. 100
Livingston, Texas 77351
(936) 327-3937
Cleveland Office
429 West Southline
Cleveland, TX 77327
(281) 592-4343
Bay City Office
3612 Avenue F
Bay City, TX 77414
(979) 244-1450
Baytown Office
4750 East Freeway
Baytown, TX 77521
(281) 421-2020
South Austin Office
2600 Via Fortuna, Ste. 400
Austin, TX 78746
(512) 327-4123
North Austin Office
4314 W. Braker Lane Ste. 215
Austin, TX 78759
(512) 200-3937
Sun City Office
1530 Sun City Blvd., Ste. 150
Georgetown, TX 78633
(512) 327-3792