
People with diabetes often have problems with the blood vessels in the eyes. If you look at the inside of a human eye, you will find the retina lining the back. This area detects light and shadows, sending visual information through the optical nerve to the brain. A healthy retina needs a steady supply of blood, rich in vital nutrients. Diabetes can cause blood vessel damage in the retina, which causes vision problems.
Diabetes can impair the ability of blood vessels to supply nutrients and oxygen to the retina. If any part of the retina becomes deprived of oxygen, it will send out a signal to get more blood supply. The body will start growing additional blood vessels to supply this much-needed oxygen. However, these new vessels, called neovascularization, do not grow normally. Instead of growing within the tissue of the eye, these blood vessels grow within a membrane along the retina’s surface. Due to changes in eye fluid or blood pressure, the membrane will contract. Squeezing this membrane can cause the new blood vessels to tear. The person will have an area of their vision darken as the blood gathers.
The blood may dissipate on its own. However, if it does not, it can trigger the formation of additional membranes which may cause the retina to detach from the inside of the eye. A detached retina can also cause dark spots in vision. This kind of eye injury requires the immediate attention of an ophthalmologist to prevent permanent damage.
Neovascularization can occur with no noticeable changes to your vision. Diabetics need to have regular eye exams to ensure that this silent condition does not cause permanent eye damage.
Diabetes can also weaken the walls of the vessels, causing them to leak. The leaking fluid can accumulate within the macula, which is the central vision spot on the retina. The accumulated fluid can cause vision to become blurry, a condition known as diabetic macular edema. It is the major cause of vision problems in people with diabetes.
Patients who have diabetes have a higher chance of developing cataracts at a younger age than most people. When a cataract forms, the person experiences clouding of the lens, which affects the light focused on the retinal surface. Diabetics may form cataracts due to ups and downs in glucose levels. This can pull water into the tissues of the lens, which makes vision cloudy.
Fortunately, there is a lot you can do to manage diabetes. The most important thing to do is get the disease under control. Changes in diet and exercise can help you keep blood sugar levels close to normal. This will help you avoid or delay complications.
You may be at risk for developing diabetes if you have the following characteristics:

The doctor needs to examine the retina. To do this, your eye will be dilated.
The doctor will be looking for changes within the retina, such as blood spots, leaking blood vessels or white areas indicating damage to the nerves. All of these changes are related to the blood vessel damage caused by diabetes. The doctor will also note if there are any abnormal blood vessels growing on the retina’s surface. With this condition, there is a significant chance that bleeding will occur. The doctor will also examine the macula for diabetic macular edema.
The good news is that many of the conditions that diabetes can cause within the eye are treatable, as long as they are caught early enough.
The current recommended treatment for the abnormal blood vessels forming on the retina is pan retinal photocoagulation, a type of laser treatment. The doctor will use the laser to destroy the places where blood vessels have closed and new blood vessels are forming. After treatment, the retina will stop signaling for new blood vessel formation. The new ones already present will start to go away. This treatment can cause complications, such as bleeding in the eye or retinal detachment. However, the Diabetic Retinopathy Study (DRS) verified that the risk of significant visual loss due to the growth of abnormal blood vessels on the retina can go down by more than 50 percent with the use of this treatment.
The same laser treatment works to treat the leaks in blood vessels that cause diabetic macular edema. The doctor may order a special angiogram to detect exactly where the leaks are occurring. This makes treatment more precise.
Visit your doctor here at Mann Eye every year. That is the most important thing you can do to prevent eye problems caused by diabetes. If you were diagnosed with diabetes, your primary care physician should have sent you to see the eye doctor right after you were diagnosed. You need an annual exam every year after that. For diabetic women who become pregnant, exams need to happen during every three months of pregnancy and then three months after the baby arrives, since the abnormal growth of blood vessels within the eyes can become worse during pregnancy.
If your primary care physician or eye doctor finds changes in the retina, you may have to go in for eye exams more than once a year. This allows the doctor to monitor the changes.
People with diabetes need to visit their physicians regularly, to keep control of the disease. Controlling blood sugar levels can decrease the risk of abnormal blood vessels growing within the eye.
Please visit our financing page for more information.
Mann Eye Institute has the latest diagnostic and therapeutic equipment and provides a comprehensive program for the diagnosis and treatment of diabetic eye disease. Focal laser surgery, or photocoagulation, is utilized to treat retinopathy at the advanced stages. A vitrectomy may also be performed to restore vision by removing hemorrhaged areas and to repair retinal detachment.
Regular eye exams, good medical management of blood sugar and blood pressure, along with timely treatment can significantly reduce the risk of visual loss and blindness. If you have any detectable retinopathy, it’s a message to practice tighter control, reduce your blood pressure, and perhaps reconsider your exercise regimen.
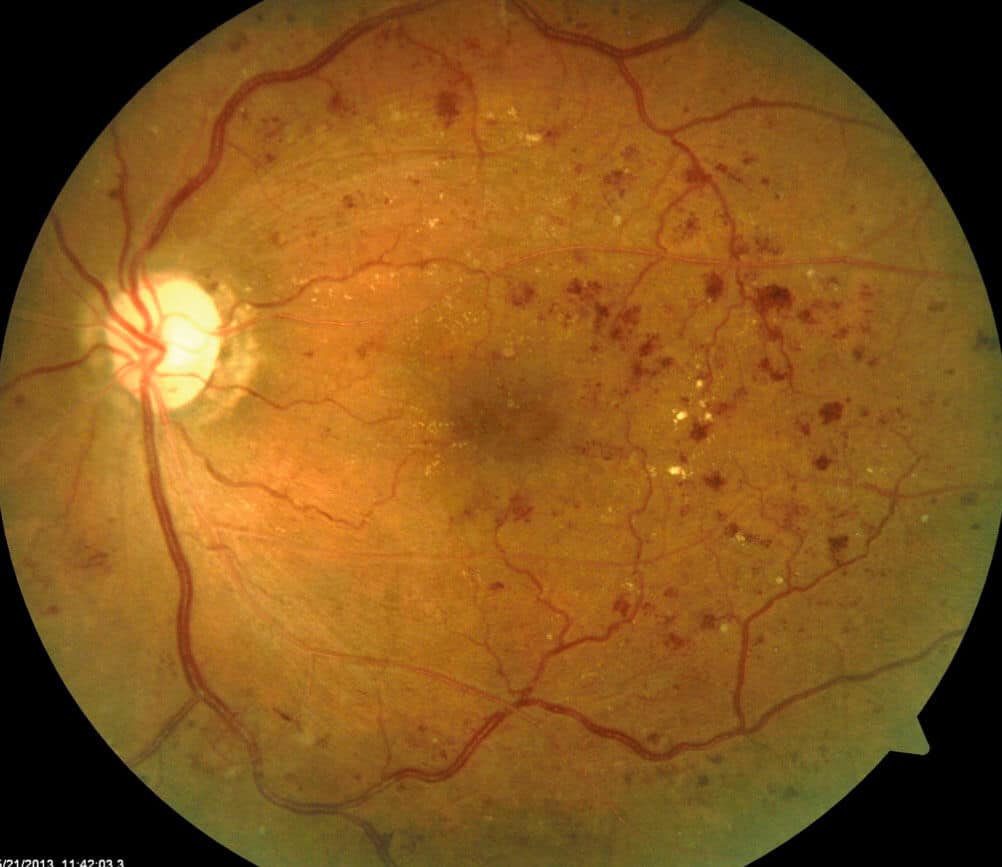
People with diabetes can develop an eye condition called diabetic retinopathy. This is when high blood sugar levels cause damage to the blood vessels in the retina. These blood vessels can swell and leak, or they can close, stopping blood from passing through. All of these changes can result in vision loss.
Diabetic retinopathy typically develops without early warning signs. The damage to the eye can occur slowly and is hard to detect without regular and accurate monitoring.
Since diabetic retinopathy rarely has symptoms in its early stages, it is possible to have diabetic retinopathy and not even know it. As the condition worsens, you may experience:
Symptoms typically affect both eyes. Because of a lack of early symptoms, it is important that if you have diabetes, you have an annual comprehensive eye exam. Your sight depends on it! The longer diabetic retinopathy goes undiagnosed, the higher the chances become that you will experience permanent vision impairment.
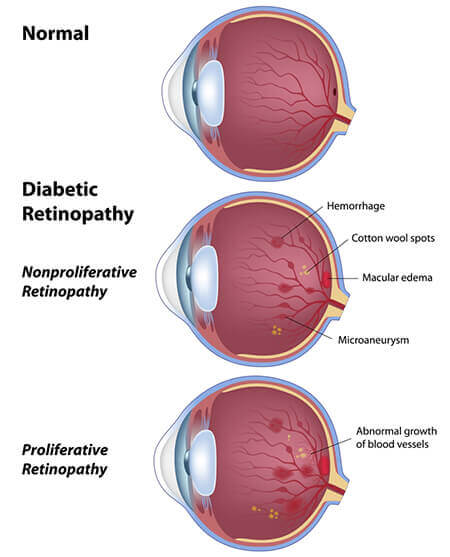
There are two main stages of diabetic eye disease:
This is the early stage of diabetic eye disease, and many people with diabetes have it. With NPDR, the weakened blood vessels can begin to leak fluid and blood. When the macula swells, it is called macular edema. This is the most common reason why people with diabetes lose their vision. Also with NPDR, blood vessels in the retina can close off, keeping blood from reaching the macula. This is referred to as macular ischemia, and can cause significant vision loss.
PDR is the more advanced stage of diabetic eye disease. In PDR, the lack of blood flow due to the number of damaged blood vessels is great enough to cause the eye to grow new blood vessels to try and help itself, a process called neovascularization. Unfortunately, these new blood vessels do not help. These fragile vessels can easily burst with minor trauma like a forceful sneeze or cough, causing the eye to fill with blood. These abnormal vessels also result in scar tissue formation that may cause the retina to detach from the back of the eye. PDR is very serious, as it can steal both your central and peripheral vision.
Treatment depends on the extent of the disease and can include:
Certain medications (injections) may help to relieve inflammation or reduce swelling of the macula, thereby slowing vision loss and perhaps improving vision.
This treatment is an injection that can help with two problems. It can reduce the number of abnormal blood vessels in the retina and can also decrease fluid. We may recommend anti-VEGF treatment in both cases of NPDR and PDR.
In certain instances, laser surgery is used to seal a blood vessel that is leaking or to stimulate the cells under the retina to absorb the leaked fluid. In some cases, more than one treatment is needed.
In the case of the more serious PDR where abnormal blood vessels have developed, we may recommend a laser procedure called panretinal photocoagulation (PRP). By using a laser to make tiny burns in the peripheral retina, we reduce the signals for the growth of the abnormal blood vessels and cause these vessels to shrink. In some cases, more than one treatment is needed.
For more severe cases of diabetic retinopathy when the eye is filled with blood or if a retinal detachment is present, vitrectomy surgery is used. Vitrectomy is a surgical procedure that removes vitreous gel, blood and scar tissue in the back of the eye. It is also used to repair retinal detachments that result from scar tissue and abnormal blood vessel growth in advanced diabetic eye disease. By removing the vitreous hemorrhage and reattaching the retina, light rays are again able to focus correctly on the retina.
If you are concerned about any diabetes-related eye problems, our experienced retina specialist, Dr. Mohsenin, will be happy to discuss potential solutions and develop an individual treatment plan for you.
The Mann Eye Institute is a leading eye care facility with sixteen locations in Humble, West Humble, Houston, Central Austin, North Austin, Sugar Land, Katy, Spring, The Woodlands, Livingston, Bay City, Pearland, Baytown, Tomball, Sun City, and Cleveland, Texas. With various locations in the Houston and Austin areas we can provide the full continuum of care, including; designer eyewear and eye care needs, LASIK eye surgery, cataract surgery, premium lens implants and dry eye treatment options. If you are seeking expert eye doctors in Texas contact us today!
The Woodlands Office
Medical Arts Center III
17450 St. Luke’s Way, Suite 100
The Woodlands, TX 77384
(281) 367-2010
Pearland Office
10223 Broadway St., Ste. J
Pearland, TX 77584
(281) 971-9332
Spring Office
2616 FM 2920 Ste. I
Spring, TX 77388
(281) 353-8300
Tomball Office
14079 FM 2920
Tomball, TX 77377
(346) 701-4029
Katy Office
750 Westgreen Blvd.
Katy, TX 77450
(281) 392-3937
Humble - Deerbrook Office
9802 FM 1960 W, Ste. 110
Humble, Texas 77338
(281) 446-9333
Sugar Land Office
6424 E. Riverpark Dr.
Sugar Land, TX 77479
(713) 580-2525
Humble - S. Memorial Office
18850 S. Memorial Blvd.
Humble, TX 77338
(281) 446-7900
Livingston Office
1601 US-59 Loop North, Ste. 100
Livingston, Texas 77351
(936) 327-3937
Cleveland Office
429 West Southline
Cleveland, TX 77327
(281) 592-4343
Bay City Office
3612 Avenue F
Bay City, TX 77414
(979) 244-1450
Baytown Office
4750 East Freeway
Baytown, TX 77521
(281) 421-2020
South Austin Office
2600 Via Fortuna, Ste. 400
Austin, TX 78746
(512) 327-4123
North Austin Office
4314 W. Braker Lane Ste. 215
Austin, TX 78759
(512) 200-3937
Sun City Office
1530 Sun City Blvd., Ste. 150
Georgetown, TX 78633
(512) 327-3792